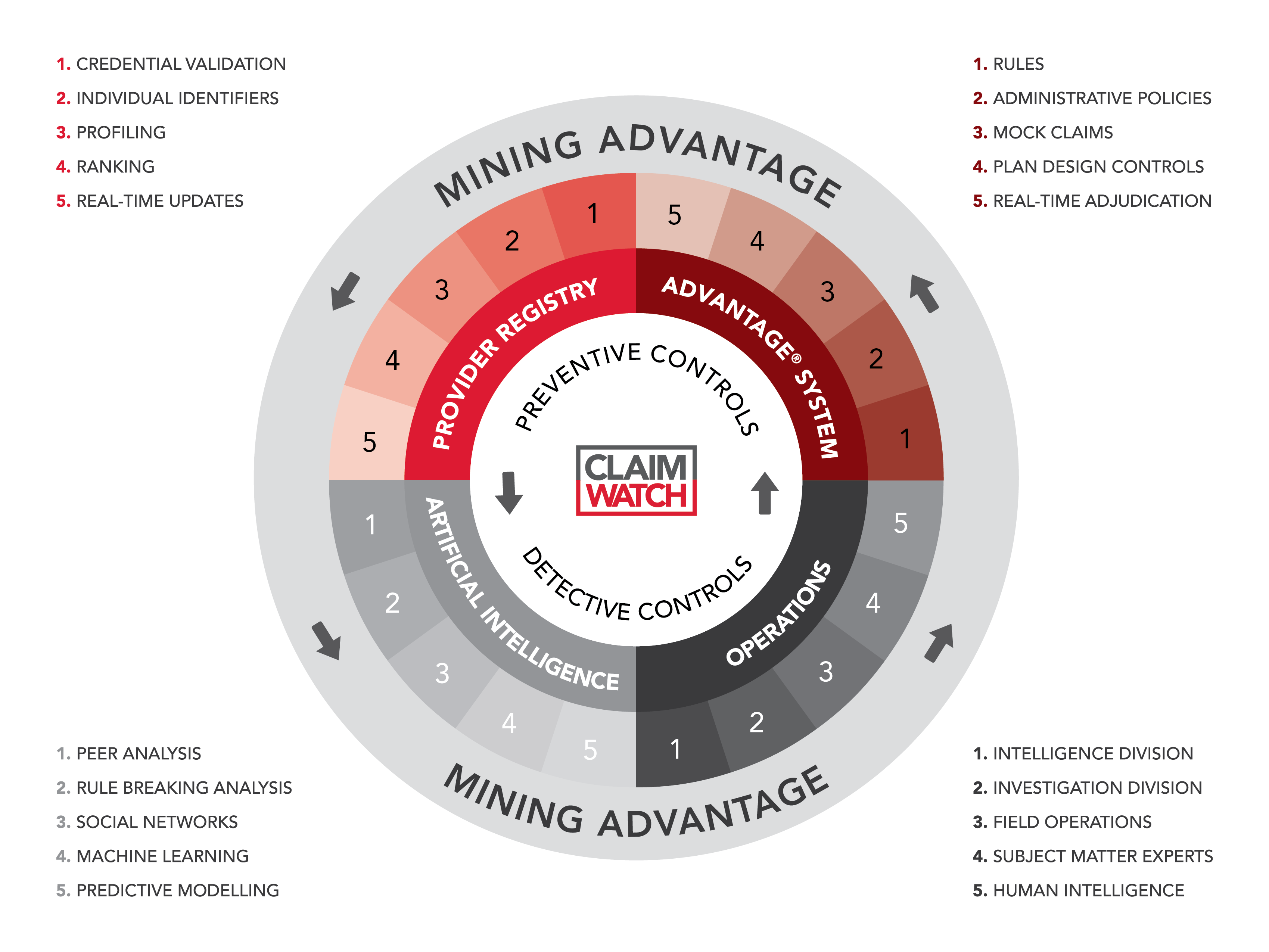
The Provider Services team is responsible for the administration and maintenance of the providerConnect® National Provider Registry which ensures health service providers have appropriate credentials and are registered on the HBM+ system before a claim is paid.
A specific list of criteria is verified for every provider accepted into the registry, including credentials, schooling, and address. The provider is then assigned a unique identification number that allows the tracking and monitoring of provider claims activity at each location they may be practising at, as well as any other provider who may be practising at the same location.
Other controls, such as provider profiling and a provider classification system, enable ongoing monitoring of provider practices and interpretation of provider claims data to identify abnormal billing patterns, service over-utilization, and excessive fees before they escalate into larger issues.
A range of prevention strategies and programs are available to help deter fraud and abuse via HBM+’s dynamic, rules-based, fully-integrated system, Advantage. Its versatility enables the automation of many Claim Watch auditing processes and applies policies and practices in real time. Through the application of rules, flagging mechanisms, or interactive messaging, Advantage can:
- Automatically pend/flag a claim so it can be reviewed by an auditor prior to reimbursement
- Send the adjudicator an interactive message to stop processing the claim so an auditor can undertake a review prior to payment
- Request additional information to support the claim, such as a lab invoice or a dental x-ray – a message on the claim statement advises the plan member/provider of the need for additional information
Smart benefits-plan design is key to avoiding fraud. A plan geared towards fraud prevention does not mean that the plan design needs to be restrictive – it just means having the right controls. Advantage was designed with a range of prevention strategies and programs to help deter fraud and abuse. These can be included or excluded, for example:
- Automated rules built into Advantage protect benefit plans against fraudulent situations like dual benefit claiming or inappropriate billing.
- Price monitoring practices such as “usual and customary” pricing guidelines are established for all eligible benefits and services to prevent over-billing by service providers and, in turn, overpayment by benefit plans.
- Built-in plan-design controls encourage plan members to access appropriate and not excessive treatments.
- Superior data-mining tools make it possible for data from every claim entered into the system to be analyzed using sophisticated HBM+ reporting tools.
At HBM+, we’re inundated by data; it comes at us in a huge volume in all forms and from all directions. And it’s utterly impossible for us humans to compile it all, let alone make sense of it. By contrast, the Claim Watch AI platform not only finds and compiles this range of data – at tremendous speeds – but also identifies patterns at a much more sophisticated level than humans can.
The AI platform also “self-educates” through machine learning, meaning the AI continuously learns as new data presents itself. And to ensure continual improvement, the results from our comprehensive investigations are fed back into the platform to establish corrective measures and enhancements. As a result, the learning curve for the Claim Watch AI platform is automatic and in real time, much faster and more sophisticated than possible for humans. Specifically, because it can amass such a broad range of data, at such high volumes, and perform very sophisticated analysis, it is able to unearth non-obvious connections, which is often where fraudulent claim activities lie.
The HBM+ Benefits Management and Investigation Services (BMIS) team is dedicated exclusively to claim investigation, audits, and fraud and abuse detection. This team consists of former law enforcement personnel, criminal intelligence officers, certified accountants, and individuals with backgrounds in the financial and public sectors. In addition, the BMIS team includes staff with extensive health care services backgrounds, including pharmacy and dental.
Every report of possible fraudulent activity is filtered through our intelligence division first to make sure that all of our sources of information are reviewed consistently and nothing gets missed. Files are then assigned to the investigative division to review the case and create a unique operation plan to address the concern. We also have field operations staff that conduct surveillance, interviews, onsite audits, and undercover investigations.